The Sangamon County Department of Public Health is asking residents to call its hotline if they think they’ve been exposed to COVID-19. But because testing is still limited by lack of supply, calling the line is no guarantee of finding out whether you actually have the disease.
Abigail House knew something might be wrong more than a week ago when she was taking her and her colleagues’ temperatures at work.
“It was a thermometer that has a beeping noise,” she said. “It has a good beep and a bad beep, and it made the bad beep noise.”
The bad beep meant House’s temp was a little elevated. She works as a nurse in a research unit at Southern Illinois University School of Medicine in Springfield. She said she went right home, and her temperature continued to climb over the weekend.
“On Sunday I learned I may have been exposed in the community,” House said. She had attended a public event with another person who later tested positive for COVID-19. She has since been home in self-quarantine.
To try to confirm if she had the disease, House started with the county health department's hotline, which referred her to Memorial Health System's respiratory clinic.
After the nurses there consulted with the Illinois Department of Public Health, which has the power to approve or deny most testing requests in Sangamon County, they eventually told her to go to the new drive-through respiratory clinic on South Sixth Street. The idea was to rule out flu or the common cold before using up a COVID-19 test.

House said she spent most of the morning on the phone or waiting to get a call back from the nurses. Her advice to others making similar calls is to be patient.
Gail O’Neill, director of the Sangamon County Department of Public Health, said she understands the screening can take a while but that getting the right information and asking questions about symptoms multiple times helps them to determine which patients qualify for a test under current rules. O’Neill said hopefully residents are in their homes and comfortable when they call, and not going to the emergency room or doctor’s office.
Drive-Through Testing
House said last Monday she took the short drive to the Sixth Street clinic in the afternoon, and there were only a couple cars ahead of her.
“[The staff] were in the over-the-head respirators, so not just a mask, but wearing something fully over their head. They first gave me a mask,” she said. They confirmed her information and that she had called ahead — in order to get screened at the clinic, residents must first call and get an appointment.
“Really quickly they did the nasal flu swab that goes way up the back of the nose,” she said.
House, who as a nurse has done a similar swab for patients before, said it was uncomfortable but not terrible. The Memorial staff then gave her instructions about keeping herself in quarantine and said she’d get results back in a few days.
It’s been about a week, which House has spent at home, limiting her contact with others and not going out. She hasn’t heard the results of her flu test or if her sample has been screened for COVID-19. House said she already called once, but she’s trying to be patient.
“While I’d like that information, I understand it might not be [a] priority at this time,” she said.
Testing Criteria
In the days since House gave her sample – testing priorities have changed. When county officials announced the first positive case here the weekend before last, the guidance was that testing would focus on those who had symptoms and had been in contact with someone with the disease or who had been travelling abroad.
Now, according to the county department of public health, which follows guidelines from the state health department, testing is focused on those who are in the hospital with unexplained pneumonia, or for people living or working in a nursing home or other group living facility where there are at least two suspected cases of COVID-19.
A spokesperson with Memorial, which collected House’s sample, confirmed the health system is following the guidelines.
Dr. Gurpreet Mander, chief medical officer at St. John’s Hospital, said his hospital is using them as well.

“If you’re sick, and well enough go home and have the symptoms, we are not recommending that they get tested,” Mander said. “That’s because of the limited supplies the state has.”
Because of that, Mander said the number of confirmed cases doesn’t give the full picture of how much COVID-19 has spread.
“I think the assumption is that it is prevalent in the community, and we have to respond to the needs of those who are sicker,” Mander said.
The lack of testing is a nationwide problem, and one that Gov. J.B. Pritzker and his administration have repeatedly complained about. Prtizker lays the blame at the feet of the federal government for not providing more tests.
In a news conference over the weekend, he said the state had requested 5,000 additional testing kits, but hadn’t received any.
Testing patients in the hospital helps physicians know how to treat them, Mander said. And it allows the hospital to take proper precautions to stop the spread among patients and medical personnel.
Mander said his focus now is on preparing for a surge in hospitalized COVID-19 patients, which modeling shows could come anytime in the next two to six weeks.
State And Private Lab Testing
The Illinois Department of Public Health reports testing nearly 9,900 people, with about 1,300 coming back positive. IDPH has three labs, in Chicago, Springfield and Carbondale, analyzing tests approved through local health departments. These numbers do not include all the tests by private companies for hospitals around the state.
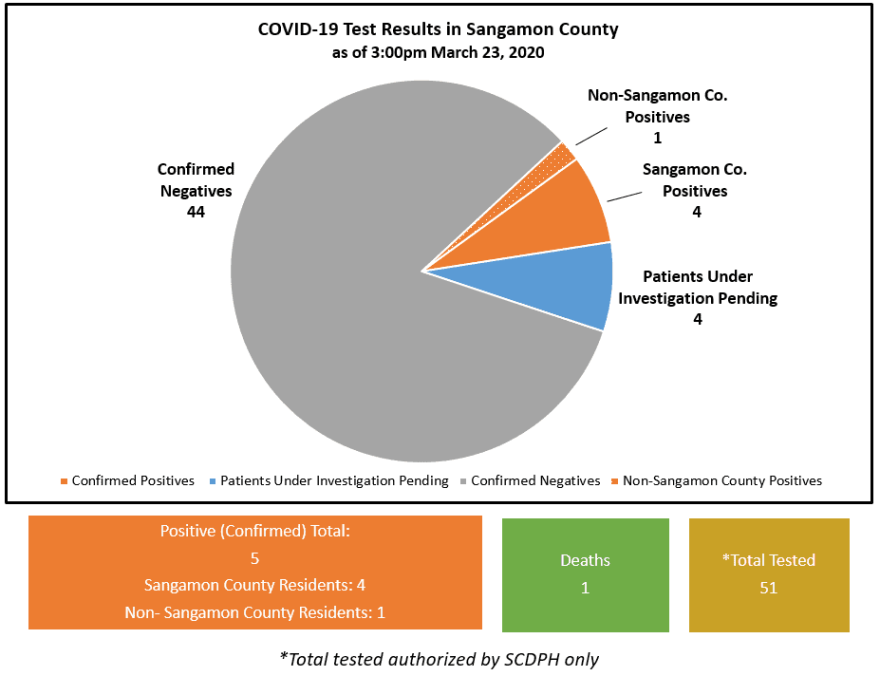
In Sangamon County, about 50 people have been approved for testing by the county public health department in the past month. Five have come back positive, including one person who died last week.
Similarly with state numbers, this does not include the testing done by private labs for local hospitals.
St. John’s has three samples pending at private labs to be tested for COVID-19, according to a spokesperson. Memorial did not give a number, but a spokesperson said they are working with the county to ensure that daily public tallies include work by public and private labs.
Memorial said the third-party testing allows them to test patients who do not fit IDPH’s guidelines.
Dr. Raj Govindaiah, chief medical officer at Memorial, told NPR Illinois last week that testing from private labs is also limited, because so many hospitals and health systems want their samples analyzed and there are only a certain number of labs set up to do that.
“We want every person whom a health-care provider thinks needs a test to get a test,” Memorial spokesperson Dean Olsen wrote in an emailed statement. But, he added: “We’re not there yet.”
According to Olsen, it can take five to seven days to get results back, in part because the lab to which they are sending samples is in North Carolina. Results from IDPH labs take about three days.
Mander and O’Neill said they’re hopeful more screening will be available in the next few weeks.
For now, House said she’ll keep staying home. To pass the time, she plays in her backyard with her shepherd-mix puppy.
“Even when it’s raining, I bet my neighbors must think I’m mad,” she said. “We’re just chasing each other in the backyard in circles. Again and again.”
As public health professionals advise, staying home is exactly what will keep people safe and slow the spread of the disease.
This story has been updated with new the number of confirmed cases of COVID-19, which is five as of Monday evening. The image from SCDPH has been updated as well.